Studying fetal hearts
November 1st, 2010
A study examining the development of fetal hearts and the placenta in pregnancy could lead to treatments to reduce the risk of complications in women with diabetes melluits.
Women with established diabetes are at fi ve times higher risk of sudden fetal death just before, during, or after labour than women without the condition.
Tragically, most deaths happen after the 32nd week of pregnancy — a stage at which, if delivered, the babies would otherwise have a very good chance of survival.
There is already evidence that the stillborn babies of diabetic women have larger hearts. Currently, there is no standard test for assessing fetal cardiac function.
This study examines how fetal hearts are working using 4D ultrasound imaging — from the amount of blood pumped through the organ to the size of the chambers of the heart — to determine a ‘normal range’ in fetal development.
By assessing these functions and comparing them to the normal range developed through this study, researchers hope to develop a tool that can predict the optimal time of delivery — either via induction or surgery — that would give the baby the greatest chance of survival.
The fetal heart study runs alongside another survey, which examines the functions of the placenta in pregnant women. The consistency of the blood flow is thought to influence fetal growth — another potential factor which affects fetal survival in diabetic women.
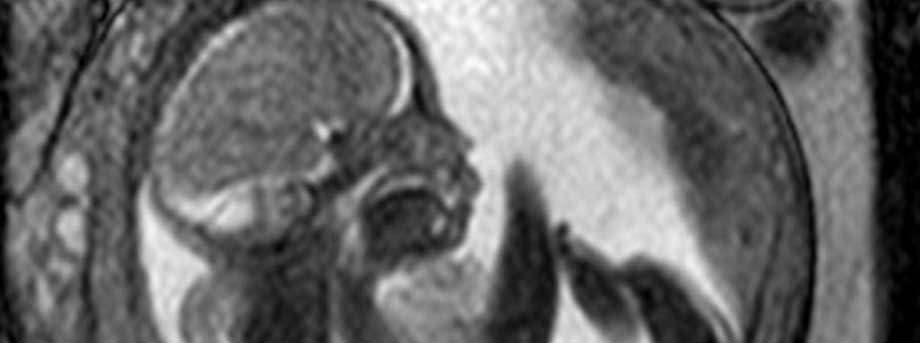
Magnetic Resonance Imaging (MRI) is being used to observe blood flow in the placenta and the baby throughout pregnancy. Researchers hope to determine whether there is a difference in placental profusion — the amount of blood fl ow — between healthy and diabetic pregnancies. The placenta is also examined post-delivery, using advanced molecular biology techniques.
Researchers in The University of Nottingham’s Brain and Body Centre and the Obstetrics and Gynaecology Division are hoping to scan 150 women undergoing ‘healthy’ — non-diabetic — pregnancies, to establish a ‘normal’ range of fetal heart size and placental profusion. Volunteers are scanned using 4D ultrasound and between 20 and 36 weeks of pregnancy. Twenty-four women will be recruited to the MRI and placental study, with scans taking place at 24 and 32 weeks.
George Bugg, Consultant in Feto-Maternal Medicine at the Queen’s Medical Centre, said: “Though it’s been observed that the hearts of fetuses in diabetic mothers can be larger than those in ‘normal’ pregnancies, a link has not yet been established between heart size, blood flow and stillbirth in these cases. By establishing a range of ‘healthy’ statistics in non-diabetic pregnancies, we can start to look at why so many diabetic pregnancies result in stillbirth, and at what we can do to prevent that.”
To volunteer for the studies you must be booked for delivery at Nottingham University Hospitals NHS Trust.
For more information or to sign up, contact Dr Ruta Deshpande at mgxrd2@exmail.nottingham.ac.uk
Tags: Brain and Body Centre, diabetes, fetal heart, Obstetrics and Gynaecology, pregnancy, research study, volunteers
Leave a Reply
Other News

Need news? See you on SharePoint
After 14 years of service, Campus News is being retired as the university’s staff news platform. […]

Roads and car parks closed for refurbishing work
As part of ongoing road improvements at the university, works will be taking place to resurface […]

